How Livestock Drug Use Impacts Human Health, Antibiotic Resistance, and the Environment
This is Part 3 of a deep dive into drug use in conventional animal agriculture.
So far, we’ve covered how these drugs became embedded in the system—and what happens after they’re used.
In Part 1, we broke down how pharmaceutical drugs became embedded in modern livestock production, and why many industrial systems now depend on them.
In Part 2, we explored what happens after those drugs are used, including how residues can persist in food within regulated safety limits. This section demonstrated that where you source your animal products from is very important. For example, conventional, non-organic milk and butter come from factory farms where there is heavy antibiotic use. “Current-use antibiotics and pesticides were undetectable in organic but prevalent in conventionally produced milk samples, with multiple samples exceeding federal limits.” (ref)

Now, in part 3 let's zoom out to look at the bigger picture: the potential implications for human health and the environment.
The Big Gap
One of the biggest gaps in this conversation is time. While natural medicinal compounds have been used in animals for centuries, the widespread use of pharmaceutical drugs in livestock production is relatively new in the context of human history.
That shift began around 1946, when researchers discovered that adding antibiotic byproducts to poultry feed significantly increased growth rates (ref). That moment marked a turning point: the beginning of routine, feed-based drug use in animal agriculture. From there, use expanded quickly.
What started as a tool for treating sick animals evolved into routine, low-dose administration, often delivered continuously through feed. By the 1950s and 60s, drug use had become deeply embedded in livestock production, scaling alongside the rise of confinement systems and industrial farming.
These changes didn’t happen separately… they grew together. As livestock systems became more concentrated and animals were raised in higher densities, disease pressure increased. Drugs helped manage that pressure, making it possible to sustain production in environments that would otherwise be difficult to maintain.
So in that sense, drug use and drug development helped enable the rise of industrial agriculture.
At the same time, there is a structured safety framework in place.
Regulatory agencies like the FDA require extensive testing of veterinary drugs, including studies on chronic toxicity, reproductive and developmental effects, carcinogenicity, and impacts on the human gut microbiome. These assessments are used to establish acceptable exposure levels, typically based on animal studies and modeled dietary intake (ref).
But these safety evaluations are not based on decades-long human studies of real-world exposure. Instead, they rely on controlled toxicology data, metabolism and residue depletion studies, and assumptions about how much of a single compound a person might consume.
Real-world exposure doesn’t happen one compound at a time.
It happens through small, repeated exposures to multiple residues across different foods, over long periods of time. And while each individual residue may fall below its regulatory limit, there is currently no widely established framework for understanding the cumulative or synergistic effects of these mixtures.
So while modern systems are effective at preventing acute harm, and the U.S. food supply is generally considered “safe”, we still don’t fully understand the long-term implications of chronic, low-dose exposure within a food system that relies on multiple pharmaceutical inputs.
Human Health Consequences
Uncertainty remains.
What we still don’t have are long-term human studies examining lifelong, low-dose exposure to pharmaceutical residues in food. We lack comprehensive data on how these compounds may affect metabolism or the gut microbiome at real-world dietary levels. And we don’t yet fully understand how they may interact with other modern exposures like pesticides, plastics, or phytoestrogens.
But this doesn’t mean we know nothing.
A growing body of research shows that veterinary drug residues can persist in animal-derived foods, and that even trace levels may have health risks (ref, ref, ref, ref). Researchers have identified several potential biological pathways through which these residues may affect the body, including toxicity, allergic reactions, disruption of the gut microbiome, and antibiotic resistance.
As one review summarizes:
“Veterinary drug residues have essential public health consequences. Toxicity, allergic reaction, antimicrobial drug resistance, carcinogenicity, mutagenicity, teratogenicity and disruption of intestinal normal flora are among the major negative impacts of these drugs in the public.” (ref)
Toxicity
Toxicity is the most well-understood risk, and the one regulatory systems are specifically designed to prevent.
Maximum Residue Limits (MRLs) are set to ensure that drug levels in food remain far below thresholds associated with acute harm. In other words, the system is built to prevent immediate or obvious toxicity.
However, at higher levels, or with repeated exposure, certain veterinary drugs have been linked to liver stress, developmental issues, and organ toxicity (ref). These effects are generally associated with exposures above regulatory limits, but they illustrate that these compounds are biologically active by design.
Allergic Reactions
Another well-documented risk is allergic reaction. In sensitive individuals, even small amounts of certain drug residues can trigger immune responses (ref). Reactions can range from mild symptoms like rashes to, in rare cases, severe and potentially life-threatening anaphylaxis (ref). This is especially relevant for drug classes like β-lactams (such as penicillin), which are known to cause hypersensitivity reactions in some people.
While these cases are not common, they are one of the clearest examples of how even low-level exposure can have real biological effects in certain individuals.
Endocrine Disruption
Another area of concern is endocrine disruption: interference with the body’s hormonal signaling systems.
Certain compounds used in livestock production, particularly hormone-based drugs, are designed to interact with biological signaling pathways. Residues of these compounds have the potential to influence hormone synthesis, signaling, or metabolism (ref).
“VDRs also disrupt endocrine and hormonal systems, interfering with hormone synthesis or activity. This imbalance increases the risk of reproductive disorders, developmental abnormalities, and chronic diseases such as obesity, diabetes, and cardiovascular conditions. Endocrine-disrupting effects include estrogen-induced feminization in males, skeletal malformations, and carcinogenic impacts on female reproductive organs.” (ref)
This is especially relevant in the modern environment, where people are already exposed to multiple endocrine-disrupting compounds through plastics, pesticides, and personal care products. Foodborne exposure may represent one additional piece of that cumulative burden.
Gut Disruption
One of the most emerging areas of concern is the impact of low-level drug residues on the gut microbiome.
The human gut is home to trillions of bacteria that play a central role in digestion, immune function, and metabolism. Antibiotics (and other drugs) are specifically designed to disrupt bacterial populations, which is why they are effective in treating infections, but also why they can have unintended effects if over used.
Research suggests that even trace levels of antimicrobial residues in food may influence the composition and activity of gut bacteria.
“The consumption of trace levels of antimicrobial residues in foods from animal origin may have consequences on the indigenous human intestinal micro flora... The broad-spectrum antimicrobials may adversely affect a wide range of intestinal flora and consequently cause gastrointestinal disturbance.” (ref)
Broad-spectrum antibiotics, in particular, have the potential to alter microbial balance, which can lead to gastrointestinal disturbances and shifts in metabolic function.
The FDA itself has identified several potential effects of antimicrobial residues on intestinal flora (ref), including:
-
> Changes in microbial composition
-
> Alterations in metabolic activity
-
> Disruption of the gut’s protective barrier
-
> Shifts in antimicrobial resistance patterns
Some researchers have even proposed that chronic, low-dose exposure to antimicrobial residues through food could contribute to broader changes in human health. One hypothesis suggests that long-term disruption of the gut microbiome may play a role in metabolic conditions like obesity (ref), though this remains an area of ongoing research.
To be clear, this is not a settled conclusion, but it reflects a growing recognition that the gut microbiome is highly sensitive to chemical exposures, even at low levels.
Antibiotic Resistance
Perhaps the most widely recognized concern is antibiotic resistance.
Antibiotic resistance occurs when bacteria adapt to survive exposure to antibiotics, making infections harder to treat. Over time, this can lead to more severe illness, increased reliance on stronger drugs, and higher healthcare costs.
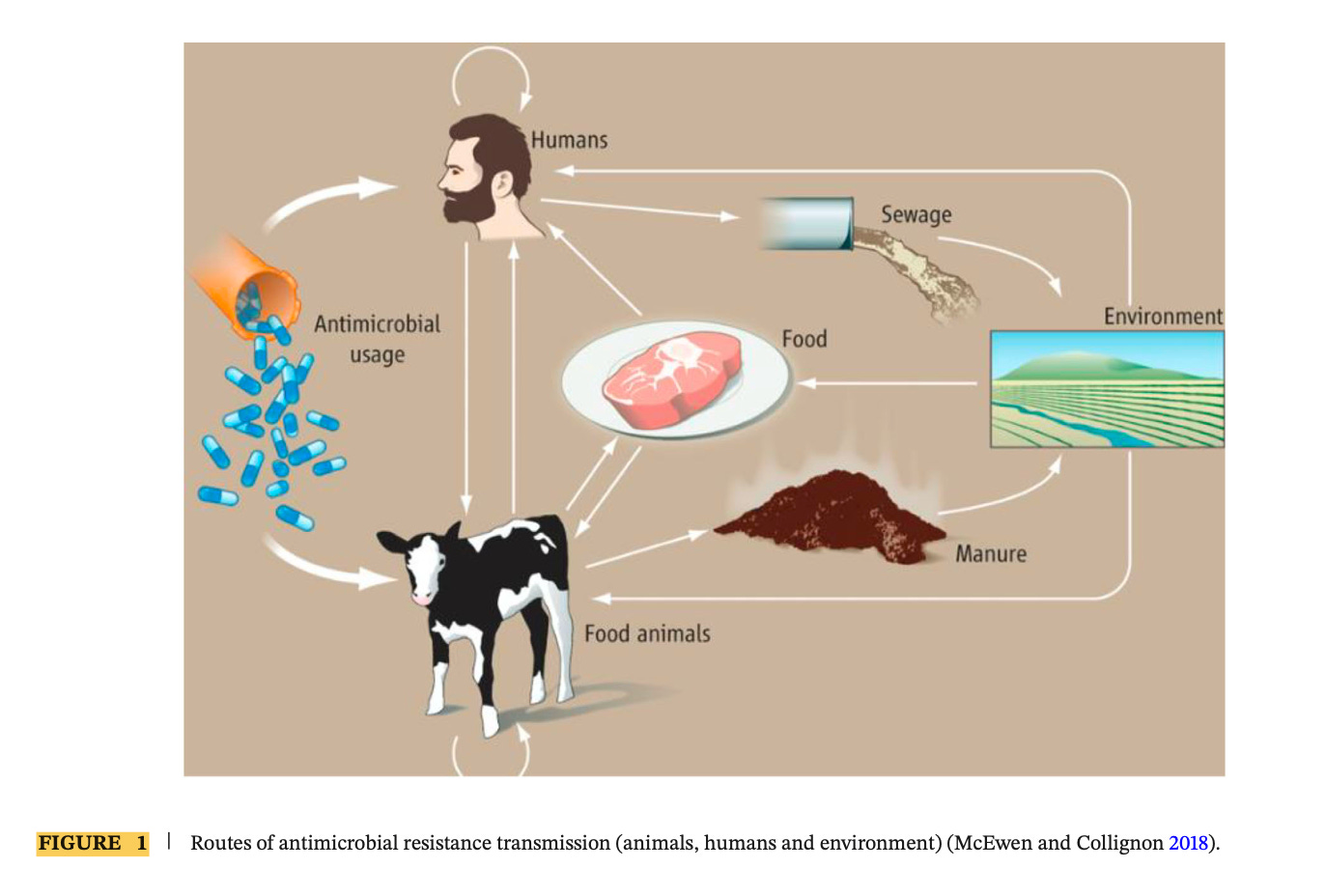
At a biological level, bacteria can strengthen their resistance by acquiring antimicrobial resistance genes (ARGs), often through gene exchange mechanisms like plasmid transfer. These genes can spread through animal populations, and move beyond the farm via manure, soil, water systems, and the surrounding environment (ref). Research shows that antibiotic-resistant bacteria can proliferate within agricultural systems and travel through multiple pathways, including contaminated water, soil, air, animal products, and even farm workers moving between environments (ref). Together, these pathways create a network through which resistance can move from livestock operations into the broader environment and, ultimately, into human populations.
In industrial livestock systems, antibiotics are often used not only to treat disease but also to prevent it and, historically, to promote growth. These uses can involve long-term, low-dose exposure, which creates conditions that allow bacteria to adapt and develop resistance. Because many of the antibiotics used in animal agriculture are the same as, or closely related to, those used in human medicine, the spread of resistant bacteria has direct implications for human health.
This is not a theoretical issue, it is a well-established and widely documented public health concern (ref, ref). Major health organizations, including the World Health Organization (WHO) and the Centers for Disease Control and Prevention (CDC), have identified antibiotic resistance as one of the most significant global health threats, with widespread antibiotic use in both human medicine and animal agriculture recognized as contributing factors. (ref)
In the United States alone, the CDC estimates that more than 2.8 million antibiotic-resistant infections occur each year, resulting in over 35,000 deaths. (ref) These infections are not only more difficult to treat, but also increase healthcare costs and complicate routine medical procedures. It is estimated that antibiotic resistant infections cost the US more than $55 billion in health expenses and lost productivity. (ref)
No, we should not rely on antibiotics. However, antibiotics are one of the most powerful tools in modern medicine. They can save lives, enable surgeries, and make advanced treatments like organ transplants possible.
But their effectiveness depends on them continuing to work.
Like any tool, overuse comes with consequences. In systems where routine use becomes necessary to maintain production, it raises important questions about long-term sustainability not just for agriculture, but for human health as well.
So this isn’t about eliminating antibiotics entirely. It’s about preserving their effectiveness for when we truly need them.
Environmental Consequences
We don’t fully understand the long-term environmental impacts of pharmaceutical drug contamination, but what we do know raises serious concerns (ref).
Many veterinary drugs are not fully metabolized by animals. Instead, a portion is excreted through manure and urine, which are then applied to fields as fertilizer or stored in lagoons. (ref) From there, these compounds can move into the environment through runoff into rivers and streams, leaching into groundwater, and discharge from livestock wastewater systems. In some cases, they can even spread through dust and air. (ref)
This creates a system where drug residues are not contained, and are continuously cycling through soil, water, and ecosystems.
And because of how modern livestock systems operate, this isn’t happening in small, isolated amounts… it’s being spread all over.
Animal manure is often viewed as a valuable natural fertilizer, rich in nutrients like nitrogen, phosphorus, and potassium. But in industrial systems, the scale is enormous.
Feedlots and CAFOs generate massive volumes of manure, which are transported and spread across agricultural land, often far from where the animals were raised.
Research estimates that 30–80% of veterinary antibiotics are excreted in manure and urine, meaning a substantial portion of what is administered to animals ends up in the environment. (ref)
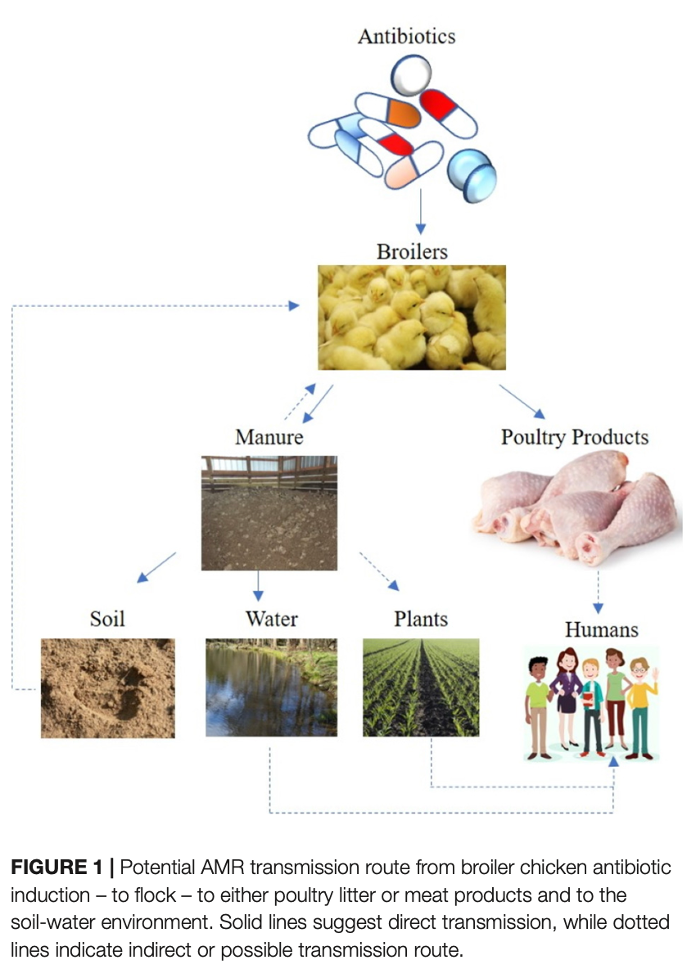
Poultry production alone generates millions of tons of litter annually, raising concerns not only about nutrient loading, but also about the spread of drug residues, antimicrobial-resistant bacteria, and resistance genes through soil and water systems. (ref, ref)
Once applied to land, these compounds don’t just stay put. Studies show that antibiotics and other veterinary drugs can migrate from soil into surface water and groundwater through runoff and leaching, becoming a non-point source of environmental contamination.
“Following land application of poultry litter, antibiotics migrate from soil through runoff, leaching, and particle adsorbed runoff potentially ending up in soil, surface water, and groundwater” (ref)
Spread of Antibiotic Resistance in the Environment
This environmental contamination contributes to the spread of antibiotic resistance beyond the farm.
Antibiotic resistance genes (ARGs have now been detected across a wide range of environments, from agricultural soils to remote ecosystems, highlighting how widely these genetic elements can spread. (ref)
In livestock systems, resistant bacteria and genes can move through multiple pathways.
Water is one key route. Studies have found antibiotic-resistant bacteria in feedlot water systems, even before animals arrive, suggesting these environments can act as reservoirs. (ref)
Airborne transmission is another often overlooked pathway. Air within and around CAFOs can contain high levels of bacteria, including antibiotic-resistant strains, allowing them to disperse into surrounding environments and nearby communities. (ref) In one study, antibiotic-resistant bacteria were detected inside vehicles driving behind poultry transport trucks, demonstrating how these microbes can move well beyond production sites. (ref)
The scale is significant. Genetic sequencing research suggests that a single gram of chicken feces can contain extraordinarily high numbers of antibiotic resistance gene copies, continuously introduced into the environment through manure. (ref)
Contamination of Water Systems
It is now well established that pharmaceutical residues are present in waterways. These compounds have been detected in rivers and streams, groundwater, wastewater, and even drinking water supplies. While some contamination originates from human pharmaceutical use, livestock production is a significant contributor, particularly in regions with high concentrations of CAFOs.
Livestock-associated antibiotics, including tetracyclines and fluoroquinolones, have been detected in rivers around the world. (ref) Other studies have found elevated levels of hormones, including estrogenic compounds, in lagoons and groundwater near large swine CAFO facilities. (ref)
Large-scale monitoring reinforces how widespread this issue is. One assessment found pharmaceutical residues in drinking water supplies serving over 41 million people across major U.S. metropolitan areas. A U.S. Geological Survey study detected pharmaceuticals and wastewater contaminants in 80% of streams sampled across 30 states, with a significant portion linked to agricultural sources. (ref)
More recent research continues to expand on these findings. A comprehensive review identified over 70 different veterinary pharmaceuticals in wastewater and surface water samples, with antibiotics being the most frequently detected and often present at the highest concentrations (ref). These findings highlight that veterinary drugs are now recognized as a significant category of environmental contaminants.
Impacts on Aquatic Life
These compounds are not inert once they enter the environment, they remain biologically active!
Studies have shown that pharmaceutical residues can affect aquatic organisms, particularly through endocrine disruption. Hormones such as estradiol and trenbolone have been linked to reproductive and developmental abnormalities in fish and other aquatic species. (ref)
Impacts on Soil and Ecosystems
It’s easy to think of soil as just dirt, but it is actually a living ecosystem, filled with microbes, insects, and organisms that play critical roles in nutrient cycling and plant health. When drug residues enter this system, they can disrupt that balance. (ref)
Antiparasitic drugs like ivermectin are a clear example. These compounds are only partially metabolized and are excreted in manure in an active form, creating direct exposure for dung-dependent organisms like dung beetles and other beneficial insects.
Research has consistently shown that these residues can have harmful effects on non-target species. Exposure has been linked to reduced survival and reproduction in dung beetles, impaired larval development, and disruption of insect communities that play a key role in nutrient cycling. (ref)
Even at low levels, effects of leached ivermectin can include impaired growth, delayed development, and reduced reproductive success (ref). Other research has shown that ivermectin residues can impair sensory and locomotor function in dung beetles, even at low concentrations (ref). And another study found that moxidectin, another commonly used antiparasitic drug, can persist in cattle dung and enter water systems, where it is toxic to aquatic invertebrates and may move through the food web. (ref)
These impacts can cascade through the ecosystem.
Dung beetles and similar organisms play essential roles in:
-
> breaking down manure
-
> recycling nutrients
-
> supporting soil microbial activity
When these populations decline, manure decomposition slows, soil structure can degrade, and the balance of the soil ecosystem can shift over time.
And this is not limited to industrial systems. Antiparasitic drugs are widely used across many types of livestock production, including pasture-based and regenerative systems.
Clearly, veterinary drugs don’t just stay in the anima, or even in the food supply.
They move through soil, water, air, and ecosystems, creating multiple pathways of environmental exposure.
While these systems are designed to support modern food production, they also introduce biologically active compounds into the environment in ways we are still working to fully understand.
And that adds another layer to the conversation, not just about food, but about the broader ecological systems we rely on to produce it.
So… What do we do with all of this?
Before discussing what you can do I think it’s important to address why I am even talking about this in the first place.
Because most people don’t even know this is happening.
Research shows that awareness of pharmaceutical drug use in livestock is low, yet the scale of use is massive and deeply embedded in how our food is produced.
A tweet went viral in 2025 when someone found out that Costco beef were vaccinated.
Well, yes. Duh! Most are!
And once you understand the system, it becomes clear: where you source your animal products from matters.
It also helps explain something many people notice, but don’t fully understand:
Why does conventionally raised meat cost less than regeneratively raised meat?
Because raising animals without routine pharmaceutical drugs requires:
-
- More time
-
- More land
-
- More management
-
- And more attention to the animal’s environment and health
You’re not just paying for the food product.
You’re paying for the system behind it.
Can the conventional system change?
On a nationwide scale, reducing pharmaceutical drug use in livestock is not simple.
Modern industrial systems are built in a way that often requires pharmaceutical inputs to function. And as long as that structure remains, drug use will remain part of the system.
There is growing interest in alternatives (such as prebiotics, probiotics, and plant-based compounds) to support animal health more naturally. (ref)
But the biggest lever isn’t a substitute product.
It’s the system itself.
Reducing reliance on pharmaceutical drugs ultimately means reducing reliance on confinement-based systems.
And at its core, this comes down to management.
You already understand this in your own life:
When you eat well, move your body, get sunlight, prioritize sleep, and manage stress—your health improves.
The same principles apply to livestock.
Changing the Food System from the Ground Up
Our modern food system has been shaped by large multinational corporations—companies like Tyson and Smithfield—alongside massive pharmaceutical companies whose scale and influence have helped define how animals are raised.
But systems like this, with billions at stake, often do not just change from the top down.
They can also change from the bottom up.
Consumer demand shapes markets. Every purchase is a signal!
Whenever you can, support farmers who are raising animals in alignment with nature and with less reliance on pharmaceutical drugs.
What We’re Doing at Nourish Food Club
At Nourish Food Club, we’re committed to doing things differently.
We’re proud to be #NeedleFree.
We call it: farming, not pharm-ing.
We don’t raise animals to survive in industrial systems, we raise them to thrive in natural ones.
That starts with management, not pharmaceutical medication.
Our approach is built on:
-
> Pasture-based, drug-free systems focused on prevention rather than intervention
-
> Animals living in alignment with natural circadian rhythms
-
> Regular exposure to sunlight, fresh air, and the natural environment
-
> Rotational grazing and mobile pasture-raised systems to reduce exposure to waste, pathogens, and parasites
-
> Diverse pastures with healthy soil that provide natural compounds to support health
-
> Lower stocking densities and smaller-scale systems (more small farms with less animals. No large confinement buildings with unnatural livestock numbers crammed in)
-
> Space and freedom to express natural behaviors: grazing, rooting, foraging
When animals are raised this way:
Stress is lower,
Immune function is stronger,
And the need for routine pharmaceutical intervention is removed.
Their basic needs are met: clean water, real food, and a healthy environment.
Why It Costs More (And Why That Matters)
Again, this kind of farming costs more.
Animals grow more slowly. They move more. They require more land, more labor, and more time. (ref)
But those differences are not inefficiencies.
They are reflections of a system designed around health, not shortcuts.
And the results show up in the final product.
Studies have shown that eggs from less-stressed hens have improved taste: “it was determined that the eggs of the no stressed hens taste better than the stressed chickens.” (ref)
Many of our Nourish Food Club members notice the difference immediately:
-
- Richer flavor and more character.
-
- Better texture.
-
- Improved digestion.
-
- More energy.
Because the reality is that animal’s environment shapes its internal biology.
And that biology shapes the food you eat.
Final Thought
We can’t fix the entire food system overnight.
But we can make different choices over time.
When you can:
-
> Support regenerative farmers
-
> Ask questions about how your food is raised
-
> Choose food you trust
Because change doesn’t just happen through policy.
It happens through people!
Get to know your local regenerative farmer.
And if you want to support what we’re building, visit Nourish Food Club, where we conveniently deliver high-quality, regeneratively raised animal products, produced without drugs, right to your doorstep.
That’s how we rebuild the food system from the ground up.